26 Aug Chronic Plantar Fasciitis? EPF!
One of the most common medical conditions I see and treat in my office is plantar fasciitis. Good ‘ole heel pain. The plantar fascia is a large ligament on the bottom of our feet that can become inflamed due to activity, weight gain, repetitive trauma, acute trauma and/or a combination of these things. The inflammation to this ligament can occur along its length on the bottom of the foot but most commonly occurs around the heel. What’s most alarming (like an alarm clock) is that patients will have sharp, acute pain to the area with the first step out of bed in the morning.
No one needs that as a wake-up call!
Plantar fasciitis, with or without an inferior calcaneal spur (bone spur on the bottom of the heel bone), is one of the most common foot problems reported to primary care physicians, orthopedic surgeons, and podiatric physicians. Fortunately, more than 90% of these cases will respond well to conservative treatment, including anti-inflammatory medications (steroidal and nonsteroidal), taping, stretching, massage/physical therapy, orthotic therapy, night splint use and injection therapy (steroids, stem cells, etc).
When conservative treatments fail, the remaining option is surgical intervention for the release of the fascia. The endoscopic plantar fasciotomy (EPF) is a minimally traumatic and minimally invasive procedure among many surgical approaches for release of the fascia. The EPF procedure does not involve removal of the calcaneal spur, because the spur does not cause the pain.
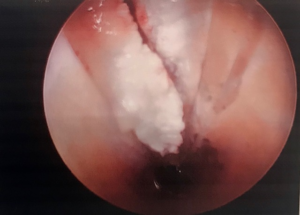
As seen with many other surgical procedures (laparoscopic, general, gynecologic, and vascular), minimally traumatic surgical techniques decrease postoperative pain and facilitate recovery. A minimally invasive procedure allows for minimization of tissue dissection and an early return to daily activities. In the case of the foot and ankle, this means an earlier return to walking, running and exercising.
With the EPF procedure, patients begin weight-bearing to tolerance within the first 24 hours after surgery wearing a pneumatic fracture boot and my patients have little to no pain immediately after surgery due to using Exparel for the nerve block. That means no narcotics or opioid medications after surgery! The bandages are changed at 4 to 6 days after surgery and sutures are removed on or about day 14. After sutures are removed, an athletic shoe can be worn as tolerated and patients can usually return to exercise about three weeks after surgery.
We don’t live in a perfect world (understatement) and like most things, complications can arise. The EPF procedure is not perfect (no procedure is); however, the rate of complication is lower and the type of complication is less severe compared with traditional heel surgery techniques. One of the complications include lateral column pain and instability (pain to the outside of the foot), possibly secondary to releasing more than two thirds of the plantar fascia. Other complications included medial arch strain with compensatory tendonitis, however when identified early and treated properly, long-term complications can be avoided.
Plantar fasciitis accounts for a large percentage of cases seen by podiatric physicians. It is in my practice. Although most cases respond well to 4–6 months of conservative nonsurgical treatment, about 10% require surgery. If conservative treatment for plantar fasciitis fails and surgery is indicated, the endoscopic (EPF) approach is superior to conventional open procedures and significantly minimizes surgical trauma resulting in an earlier return to regular activities with fewer complications.
Minimization of tissue dissection and the earliest return to daily activities are goals of any surgical procedure. Mission accomplished with the EPF procedure!
You don’t need to live in pain when you don’t have to! If your morning wake-up call includes a sharp pain to your heel, give me a call. It’s always my number one priority to helping you place your best foot forward, again!

