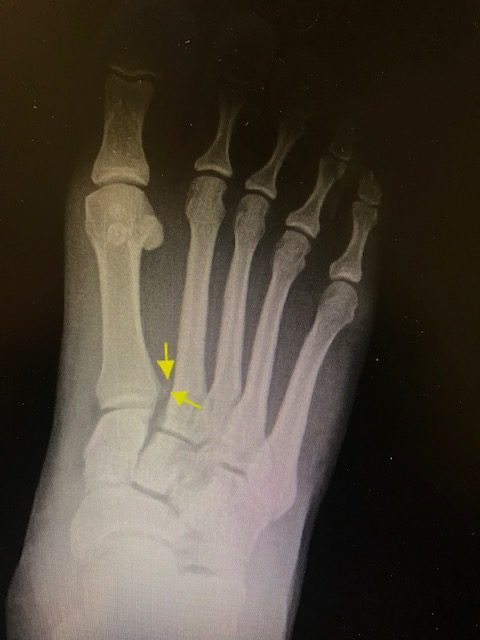
20 Jun Foot Sprain? Nope!
If you’ve been diagnosed with a “foot sprain” and you’re still not walking correctly, you may have something more serious going on. Many times a foot sprain is a more serious condition known as a Lisfranc (midfoot) injury. The Lisfranc injury is very often mistaken for a simple sprain especially if the injury is the result of a straightforward twisting type fall. Patients are often told they can simply “walk the injury off,” however patients will often continue with pain and swelling.
The midfoot is just where it sounds, the middle of the foot. It’s comprised of a cluster of small bones held together by ligaments that help form the arch of the foot. The metatarsals (long bones) extend from this cluster of bones, and in a twisting fall all of these bones can shift and become dislocated. The arch of the foot is comprised of three arches, not one. There is the medial, lateral and transverse arch and the middle cuneiform bone acts as the “keystone” for the transverse arch. So, the midfoot is critical in stabilizing the transverse arch and if disrupted leads to pain, instability and difficulty walking.
This cluster of small bones making up the midfoot is known as Lisfranc joint. The area is named after French surgeon Jacques Lisfranc de St. Martin (1790 – 1847) who served in Napolean’s army during the 1800’s. In fact the Lisfranc joint, Lisfranc ligament, Lisfranc amputation and Lisfranc fracture are all named after him. He first described the Lisfranc fracture when horseback riders would fall with their feet caught in the stirrups of their saddle. Ouch!
Lisfranc injuries can be simple or complex. There are various classification systems for this injury and the injury can range from a simple disruption to a single joint to a complex injury that disrupts several of the joints of the midfoot.
Patients will most typically have pain and swelling to the top of the midfoot. The pain is made worse with walking and standing, and patients will have pain to the midfoot when pushing off. Bruising to the bottom of the foot is highly suggestive of a Lisfranc injury.
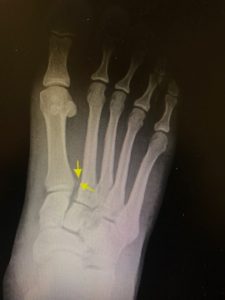
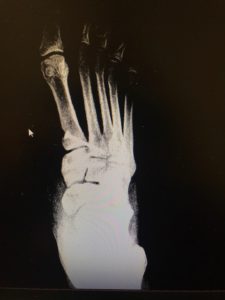
Your foot and ankle specialist will want to obtain x-rays of your feet, and I do mean both feet. A good initial evaluation will involve comparative weightbearing x-rays of both feet. The ability to compare one foot to the other will allow your podiatrist to evaluate the midfoot and look for a diastasis between the base of the first and second metatarsal. Most times a MRI will be ordered to further evaluate for soft tissue damage to the midfoot and to determine if there is a disruption to Lisfranc ligament.
Treatment for Lisfranc injury depends on the severity of the pathology. Nonsurgical treatment is indicated if there are no fractures and the ligaments are not completely torn. Surgery is always recommended for injuries where the bones have fractured and/or there is abnormal positioning (subluxation) of the midfoot joints. The goal of surgical intervention is to realign the bones and joints correctly (reduce) and to create a strong repair for walking.
If internal fixation is required, screws will be placed to reduce the deformity that was created by the trauma. Screws will be placed across the joints that normally have some motion and over time the hardware may suffer metal fatigue and break. Surgery can still be successful even if some of the hardware fails. Depending on the nature of the injury and the time that the midfoot has remained undertreated, an arthrodesis (fusion) to some of the joints of the midfoot may be required.
For recovery, patients are typically kept non-weightbearing for four weeks followed by partial- to full-weightbearing for an additional four weeks. Patients will be stepped down from their fracture boot to an ankle brace with supportive footgear, and may begin limited weightbearing exercise twelve to fourteen weeks after surgery.
If you’ve fallen off your horse and had your foot twisted in the stirrup or you continue with unexplained midfoot pain, come and see me. You may have a Lisfranc injury (say it using your best French accent!).
You don’t need to live in pain when you don’t have to! If the pain and swelling persists, give me a call. It’s always my number one priority to helping you place your best foot forward, again!

